What is heart valve surgery?
Heart valve surgery is a procedure where the surgeon enters the chest cavity and either replaces or repairs the faulty valve. This is almost always performed on a heart-lung bypass machine. The surgeon can access the heart via various routes but most commonly this is done by making an incision down the front of the chest and opening the heart via the breastbone.
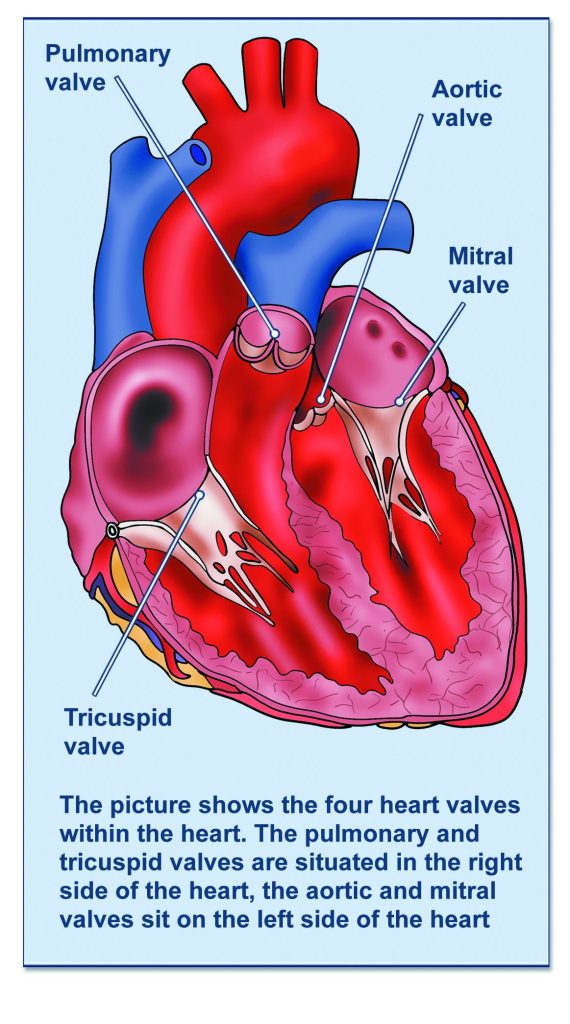
What are the benefits of heart valve surgery?
Once you develop heart related symptoms with severe heart valve disease, your outlook is much improved following heart valve intervention. The aim of a heart valve replacement or repair operation is to give you a normally functioning heart valve. This should not only improve your symptoms but should improve your outlook, prognosis and quality of life.
What are the risks of heart valve surgery?
In the vast majority of patients the benefits (both in terms of symptom improvement and survival) of heart valve surgery outweigh the risks.
Heart valve surgery is however a relatively large surgical operation and your surgeon will discuss the risks and benefits with you before you sign a consent form.
The risk of surgery is reduced by ensuring your health is as good as possible prior to your operation. You can do this by taking your medication as prescribed, keeping your weight within a healthy range, stopping smoking and ensuring you are active. Complications will vary according to the type of procedure and your personal medical history.
Complications quoted to you by your surgeon may include not surviving the operation, bleeding, infection, stroke or mini stroke, abnormal heartbeat (arrhythmia) and kidney problems. They will also advise you that the heart valve repair may not last your lifetime, especially if you are not having a mechanical valve replacement operation.
It is often helpful to write any questions you have prior to your consultation with the surgeon and take them with you to the outpatient clinic.
What tests will I need in anticipation of heart valve surgery?
In order to assess your suitability for surgery you may be sent for further tests. These often include:
Transoesophageal echocardiogram (TOE)
This is a day case procedure which takes place under sedation. A probe is passed into the gullet and detailed pictures of the heart are obtained using ultrasound.
Angiogram
This a day case procedure to assess whether there is any furring up of the heart arteries. A tube is inserted under local anaesthetic into the artery in the wrist which travels to your heart. An injection of x-ray dye shows the heart arteries in detail.
Lung (pulmonary) function tests
These are designed to assess how well your lungs are working. You will be asked to carry our various breathing exercises which measure different aspects of your lung function.
Carotid Ultrasound
An ultrasound scan of the neck arteries to look for blockages.
Chest X-Ray
Chest CT
Cardiac MRI
Preparing for surgery
Ahead of surgery
Make sure you have had a dental check within the last six months. Good oral hygiene is important, because an infection around the teeth or in the gums can spread to the replaced or repaired heart valve. This would be difficult to treat and often requires repeat surgery.
If you are on benefits you will not be available for work during your hospital stay and recovery. You will need to inform the benefits agency.
Your surgeon will let you know which medications to stop and when.
Expect to be in hospital for about a week, or longer if you have other conditions that might extend recovery.
Choose clothes for your stay which are loose and will not cling to your chest. Front opening tops are also much easier to put on after surgery and make sure the buttons are easy to do up.
If you wear a bra, wearing one immediately after surgery helps the wound to heal and is highly recommended. Bras should be front-clasping. A purpose-designed surgical bra is better still. There are excellent purpose-designed surgical bras which have soft padded front-fastening clasps. (Such as BHIS Post-operative Cardiothoracic Support Bra, www.bhisbra.co.uk Tel: 0800 279 2050). Ask your nurses for details well before your admission to hospital.
Prepare the house in readiness before going in to hospital. Make sure that the fridge and freezer are well-stocked with food, including ready meals.
If your favourite chair is low, you may find it difficult to rise from sitting in the first 2 weeks or so. Think about replacing your low chair temporarily with a higher chair with arms.
Most people feel weak and lacking in energy after going home. You’ll need to be looked after usually by a spouse or partner, or consider staying with a friend or relative for a week or two.
On admission
You will usually come into hospital the day before surgery. Sometimes you may need to be admitted for longer if there are tests still needed or if your condition needs to be stabilised or changes to medication are needed (for example changing from warfarin to heparin).
You will be ‘clerked in’ by a nurse who will assess many things like your risk of falling or whether you might have memory problems or be at risk of delirium (a form of confusion) after surgery.
The hospital staff will direct you in ways of reducing wound infections like checking for and treating MRSA colonisation (MRSA is methicillin resistant Staphylococcus aureus which can colonise the skin and nasal passages and cause wound or blood infections which are difficult to treat). Do not shave the operation site ahead of going in. The nursing staff will clip any hairy skin in the area of the incision whilst you are in. You will probably be asked to shower the day before and on the day of surgery with an antibacterial wash.
You should expect to see someone from your surgeon’s team and an anaesthetist who will check whether you have any questions and also that there have been no changes in your condition since you were seen in the outpatient clinic. If you are having a TAVI you will see someone from your interventional cardiologist’s team. If you are in a teaching hospital you may be visited by a medical or nursing student.
Sadly, operations do sometimes have to postponed. Emergencies must take precedence over more stable cases. If there are no vacant recovery or intensive therapy beds it might not be safe to proceed with your surgery. This could happen during a flu or other epidemic. Postponing surgery is a major stress; no surgeon ever does this lightly.
After surgery
The first few hours after surgery
Pain is not usually a problem because of the strong pain-killing medicines used.
It is common to be a bit confused and to lose memory for recent events. This usually recovers quickly within a day or two.
You will have:
- Low-adhesive plasters over your wounds.
- Thin tubes or drains inside your chest cavity.
- Intravenous lines for a day or two.
- A urinary catheter usually for a few hours
Often pacing wires are attached to the outside of the heart and brought onto the skin. These may be attached to an external pacing box or may be left for use in case the heart rhythm slows and pacing is needed.
Possible complications
Sometimes fluid continues to leak from the drains as the anaesthetics from the operation wear off and the blood pressure rises. Minor oozing of blood at the end of surgery can turn into more severe bleeding, requiring vessels to be tied off or oozing areas to be cauterized. It may then be necessary to go back to theatre to find the source of the leak. This occurs in about 3 in 100 cases.
A chest infection may complicate recovery, especially if there is preceding lung disease. Wound infections are uncommon but more likely in people who are overweight or have diabetes.
Abnormal rhythms and fast heartbeats are common, and easily treated with drugs.
There is a small chance of the conducting tissues of the heart being damaged leading to the need to implant a permanent pacemaker. For mitral valve replacements the chance overall is 1 in 10 and for aortic valve replacements it is 3 in 100. The chance is higher for TAVI, 5 in 100 for some balloon-expandable valves and 1 in 5 for self-expandable valves.
On the ward
The surgical plaster over your wound will be removed by a nurse usually on the 4th or 5th day after surgery.
It’s important to take a daily shower. Nurses will advise you about showering your wound. You should wash your hands regularly, about 10 times a day, to avoid contaminating your skin.
The drains in your chest will be taken out one by one between the first to the 5th day after surgery. If you have pacing electrodes these will usually be removed on the 5th day. The sensation of having the drains and electrodes removed is very strange, but not usually painful because you will be given pain-relief before the procedure. Be sure to ask about this to avoid discomfort.
You will be helped to sit in a chair the day after your operation. Physiotherapists will visit you to start some basic movements and exercises, if needed.
You’ll be given a rolled-up towel to hold tight to your chest and asked to cough to expand the lungs and clear secretions. This may seem too much of a challenge but it usually turns out much easier than you imagined.
You’ll be encouraged to walk to the bathroom and around the ward when you’re fit enough (usually by the third day after your operation).
It’s important to eat well. If your appetite is poor, ask your partner or friend to bring your favourite treat in to tempt you.
Following discharge
In the day or two before discharge you may have an echocardiogram to check that the replacement valve is functioning well and that there is no unexpected problem like fluid around the heart.
However if you are well the echocardiogram may not be done until your first postoperative visit. This is needed to show the ‘fingerprint’ of the valve in terms of the appearance of the valve and the Doppler signals. Every valve is individual and it is important to have a baseline against which to compare future echocardiograms.
On the day of discharge you will be seen by your surgical team to check that all is well. You will also receive your discharge medication and a summary of your hospital stay.
You may need a wheelchair to take you to your transport.
You should have cushions around you in the car and plenty of padding between your chest and the seatbelt.
At home
The scar will be red and a little raised at first but this will gradually resolve. People who have a severe keloid reaction to ear-piercing (a warty lump at the site of the piercing) may notice a similar effect over part of the chest wound.
A little oozing of thin fluid from the wound is normal and should dry up within a week or two. An infection shows itself as a reddening of the skin around the scar, discomfort and yellow, green or brown pus. This is not common but if you notice any of these you should immediately contact your GP.
Mild clicking of the sternotomy is common and will resolve quickly.
Wash your hands frequently.
Do not touch the wound and do not fiddle with any stitches. These are usually dissolvable, but an appointment will be made with the local Practice Nurse if any require removal.
You should not soak the scar in a hot bath until the wound has fully healed which is after about four weeks. Until then wash the area around the wound with liquid soap without rubbing. Dab dry with a soft towel. Do not use ointments.
The skin wound is half way to being healed at weeks after the operation and fully healed by 6 weeks. After this you can use a seat-belt and start driving.
The breast bone is held together firmly by stainless steel wires as it heals so it cannot burst but you should still avoid too much lifting of heavy weights like large saucepans for 3 months because this will be sore. Discomfort like a bruised or raw feeling in the chest is normal for the first few weeks especially if the left internal mammary artery has been used as a graft for a blocked coronary artery.
You may notice a tendency to “hunch” as a protective reflex around your chest wound. This can become a habit, and if it is still evident at six weeks it may be advisable to ask a physiotherapist about appropriate remedial exercises.
Some people like to have advice about when it is safe to resume sex. The answer is when you feel like it, usually after 6 weeks.
Most people gradually improve and aim to build up towards normal activity over the next 6 to 8 weeks.
We usually advise returning to work after 3 months or at minimum after 2 months if you have a relatively sedentary job.
Cardiac rehabilitation helps you get back to as full a life as possible. It is an individualised programme usually made up of a mix of exercise and education sessions, relaxation training and psychological support. Nurses may do physical checks and will offer advice, for example about stopping smoking or weight control. Most programmes offer one or two classes a week and run for 6 to 12 weeks.
